What Is a Cephalohematoma?
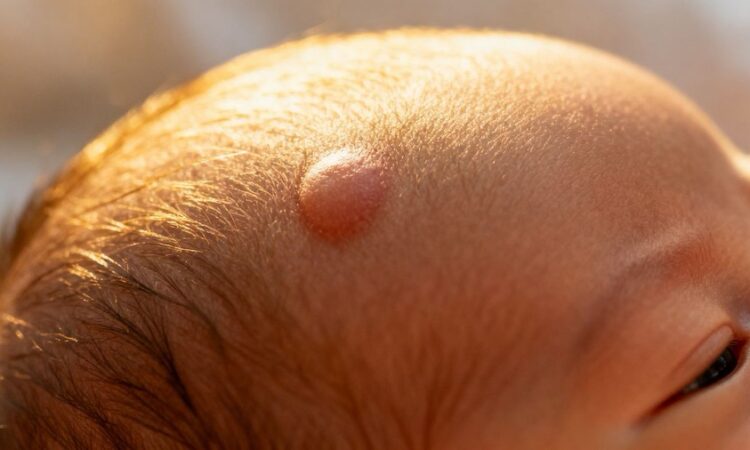
A cephalohematoma is a collection of blood that forms between the scalp and the skull of a newborn. It’s essentially a type of bruise that happens on the outside of the skull, not within it. This condition arises when the delicate blood vessels in the baby’s scalp rupture, usually due to pressure experienced during labor and delivery. The blood then pools in this space, creating a noticeable lump.
How Common Is This Condition?
Cephalohematomas are not exceedingly rare. They can occur in about 1% to 2% of all births. The likelihood increases significantly with certain delivery methods. For instance, assisted deliveries, such as those involving vacuum extractors or forceps, raise the incidence to around 3% to 4%. While it might sound concerning, most cephalohematomas are considered benign and resolve on their own.
The Physical Appearance of a Cephalohematoma
The most obvious sign of a cephalohematoma is a raised bump or swelling on the baby’s head. This lump typically appears within the first day or two after birth and might seem to grow slightly larger over the next few days. Initially, the area feels soft to the touch. Over time, a few things can happen:
- Calcification: The pooled blood can start to harden, making the lump feel firmer.
- Resorption: The baby’s body gradually reabsorbs the blood.
- Appearance Change: As the blood is reabsorbed, the center of the lump may flatten out before the edges, creating a “crater-like” or ring appearance. This is often a sign that healing is progressing well.
Cephalohematoma Causes And Risk Factors
A cephalohematoma, which is a collection of blood under the scalp, typically forms due to pressure or minor trauma experienced by the infant’s head during the birthing process. While it can occur in any vaginal delivery, certain circumstances significantly increase the likelihood of its development.
Pressure During Labor and Delivery
The journey through the birth canal can be challenging for a newborn. The baby’s head may encounter significant pressure, especially when it comes into contact with the mother’s pelvic bone. This constant pressure, combined with the force of uterine contractions, can cause delicate blood vessels on the scalp to rupture, leading to bleeding and the formation of a cephalohematoma. Prolonged or difficult labor, often characterized by weak contractions or a mismatch between the baby’s head size and the mother’s pelvis, heightens this risk.
Assisted Delivery Methods
When a vaginal delivery requires intervention, the use of instruments like vacuum extractors or forceps becomes more common. These tools are designed to help guide the baby out, but they can exert considerable force on the infant’s head. Even when used with care and skill, this external pressure can damage the small blood vessels beneath the scalp, making cephalohematoma a more probable outcome. The risk is notably higher when these methods are employed compared to unassisted births.
Infant Size and Position
Larger-than-average babies, a condition sometimes referred to as fetal macrosomia, face greater challenges navigating the birth canal. Their size can lead to increased pressure and friction during delivery. Additionally, an abnormal fetal position, where the baby is not ideally oriented for birth, can complicate the labor process, potentially prolonging it and increasing the chances of head trauma.
Multiple Births
Carrying and delivering more than one baby presents unique challenges. The process of delivering twins, triplets, or other multiples can be more complex and may involve a higher incidence of interventions. This increased complexity can, in turn, raise the risk factors associated with cephalohematoma for one or more of the infants involved.
Recognizing the Signs and Symptoms
When a baby is born, parents and medical staff are naturally focused on the infant’s overall health. However, certain conditions can arise that require careful observation. Cephalohematoma, a collection of blood under the scalp, is one such condition. While often harmless, recognizing its signs is important.
The Characteristic Bump
The most apparent sign of a cephalohematoma is a swelling on the baby’s head. This isn’t just any bump; it typically presents as a firm, raised area that is well-defined. Unlike some other types of swelling that can spread across the skull, a cephalohematoma is usually confined to the area over a single skull bone. It might not be visible immediately after birth, sometimes taking a day or two to fully develop as blood accumulates. This swelling can vary in size, from a small lump to a more significant raised area.
Changes in the Hematoma Over Time
As the body begins to heal, the cephalohematoma will change. Initially, it might feel soft and somewhat spongy, but over several weeks, it can become firmer. This is because the blood clot starts to organize and may eventually calcify, meaning it hardens. In some cases, a slight indentation or “crater” might form as the area heals, which is generally a positive sign. The entire process of resolution can take weeks to months, and it’s important to monitor its progression.
Subtle Internal Indicators
Beyond the visible swelling, there can be other, less obvious signs that a baby might have a cephalohematoma or be experiencing complications. These can include:
- Feeding difficulties: The baby may seem uninterested in feeding, have trouble latching, or tire easily during nursing or bottle-feeding.
- Lethargy: The infant might appear unusually sleepy, less responsive than normal, or generally listless.
- High-pitched crying: An unusually sharp or high-pitched cry can sometimes indicate discomfort or pain.
- Jaundice: A yellowing of the skin and the whites of the eyes can occur if the breakdown of red blood cells from the hematoma overwhelms the baby’s liver’s ability to process bilirubin.
- Anemia: In rare cases, significant blood loss into the hematoma can lead to anemia, characterized by paleness, rapid heartbeat, and fatigue.
Potential Complications of Cephalohematoma
While many cephalohematomas resolve on their own without issue, it’s important to be aware that complications can arise. These can range from mild to severe, and in some instances, may indicate a need for further medical attention or raise questions about the delivery process.
Anemia and Jaundice
One potential complication stems from the blood that collects within the cephalohematoma. As this blood is reabsorbed by the baby’s body, it can lead to an increase in bilirubin levels. Bilirubin is a byproduct of red blood cell breakdown, and elevated levels can cause jaundice, a yellowing of the skin and the whites of the eyes. In more significant cases, the loss of blood into the cephalohematoma can also lead to anemia, characterized by a low red blood cell count. This can make the baby appear pale and lethargic. Severe jaundice, if left untreated, can potentially lead to kernicterus, a serious form of brain damage.
Infection and Its Risks
The collection of blood under the scalp can, in rare circumstances, become a site for infection. If bacteria enter the cephalohematoma, it can lead to localized infections. In more serious scenarios, this infection could spread, potentially causing sepsis (a body-wide infection) or meningitis (an infection of the membranes surrounding the brain and spinal cord). These are serious conditions that require immediate medical intervention. Prompt monitoring for signs of infection, such as increased redness, warmth, or fever, is vital.
Associated Skull Fractures and Brain Bleeds
It’s not uncommon for a cephalohematoma to occur alongside a skull fracture. Studies suggest that roughly one in four babies with a cephalohematoma may also have a linear skull fracture. While many of these fractures are simple and heal without intervention, they do warrant careful medical evaluation. In more severe cases, the trauma that caused the cephalohematoma and fracture could potentially lead to bleeding within the skull or increased pressure on the brain. Recognizing signs of distress, such as unusual irritability, lethargy, or seizures, is important, as these could indicate a more serious underlying injury that requires prompt medical attention.
Diagnosis and Medical Evaluation
Initial Post-Birth Assessment
When a baby is born, a thorough physical examination is standard practice. This initial assessment by healthcare providers is designed to check for any immediate health concerns, including visible signs of trauma or unusual swelling on the head. The medical team will carefully feel the baby’s head, noting the size, location, and texture of any bumps. They’ll also observe the baby’s overall condition, looking for signs like lethargy or feeding difficulties that might accompany a cephalohematoma. This early evaluation is key to identifying the condition promptly.
When Further Evaluation Is Needed
While many cephalohematomas are identified during the initial newborn check, further investigation might be necessary in certain situations. If the swelling appears unusually large, if it doesn’t seem to be shrinking over the first few days, or if the baby shows signs of distress, doctors will likely recommend more tests. These might include:
- Blood Tests: To check for anemia, which can happen if a lot of blood collects in the cephalohematoma, or to assess bilirubin levels, as cephalohematomas can sometimes contribute to jaundice.
- Imaging Scans: Techniques like X-rays, CT scans, or MRIs can provide detailed views of the head. These are particularly useful for ruling out associated injuries, such as skull fractures or any potential bleeding within the brain, and to get a precise measurement of the hematoma.
- Head Circumference Measurements: Regular monitoring of the baby’s head size can help track the growth or resolution of the swelling, providing important data for the medical team.
Managing and Treating Cephalohematoma
When a baby is born with a cephalohematoma, it can be a cause for concern for parents. However, in most cases, this condition resolves on its own without the need for extensive medical intervention. The primary approach often involves careful observation and allowing the baby’s natural healing processes to take effect.
The Role of Watchful Waiting
For many newborns, a cephalohematoma is a temporary condition that requires no active treatment. The body gradually reabsorbs the accumulated blood over a period of weeks to months. During this time, healthcare providers will typically monitor the size and appearance of the swelling. The key is consistent observation to ensure the hematoma is not worsening or showing signs of complications.
- Regular Check-ups: Follow-up appointments with the pediatrician are important to track the healing progress.
- Monitoring for Changes: Parents should be aware of any significant changes in the bump’s size, color, or texture.
- Patience: Understanding that healing takes time is vital, as rushing the process is usually unnecessary.
When Medical Intervention Is Necessary
While watchful waiting is common, there are instances where medical intervention might be considered. This is usually reserved for cases where complications arise or the hematoma is exceptionally large. In rare situations, a cephalohematoma may apply excessive pressure to the skull, potentially causing abnormal bone development, though this is uncommon. If complications like severe anemia or jaundice develop, or if there’s a suspicion of infection, medical treatment will be initiated. In very rare cases, a doctor might consider draining the hematoma, but this is not a standard procedure and carries its own risks.
Home Care Considerations
When a baby has a cephalohematoma, home care primarily focuses on comfort and continued observation. There are no specific treatments to apply to the bump itself. Instead, parents should focus on:
- Gentle Handling: Be mindful when handling the baby, especially around the affected area.
- Following Medical Advice: Adhere strictly to the pediatrician’s instructions regarding follow-up appointments and any signs to watch for.
- Seeking Prompt Attention: If any concerning symptoms arise, such as fever, increased swelling, or changes in the baby’s behavior, contact a healthcare professional immediately. Early detection of issues like cephalohematoma infections is important for timely treatment.
Long-Term Outlook and When to Seek Legal Counsel
Typical Healing Progression
Most cephalohematomas resolve on their own without lasting issues. The swelling typically starts to decrease within a few weeks, and the blood collection usually disappears completely within two to three months. In some instances, the body may reabsorb the blood more slowly, and calcification can occur along the edges of the hematoma, leading to a hardened rim that might persist longer. This gradual resolution is the most common outcome. However, it is important for healthcare providers to monitor the healing process to ensure no complications arise.
Identifying Potential Medical Negligence
While cephalohematomas often occur without any fault, certain situations may suggest that medical negligence played a role. If the hematoma is unusually large, develops rapidly after birth, or is associated with other signs of trauma, it warrants closer examination. Delays in diagnosis or failure to recognize and manage complications like severe anemia or jaundice can also be indicators. If a baby’s condition worsens significantly or fails to improve as expected, it might point to issues with the care provided during labor and delivery. Understanding your legal options is a key step if you suspect negligence.
Understanding Your Legal Options
If you believe that medical errors contributed to your child’s cephalohematoma or its complications, seeking legal counsel is advisable. A birth injury attorney can assess the specifics of your case, including the medical records and the circumstances of the birth. They can help determine if the care provided met the accepted medical standards and if any deviations led to harm. Legal action can help secure financial compensation to cover:
- Ongoing medical treatments and therapies
- Specialized care needs
- Lost future earning potential
- Pain and suffering
Consulting with experienced legal professionals can provide clarity on your rights and the potential for seeking justice for your child.